OVERVIEW OF COMMUNITY REINTEGRATION
Community reintegration “involves return to participation in desired and meaningful activities of daily living, community interests and life roles following a stroke event. The term encompasses the return to active community living and contributing to one’s social groups and family life” (Cameron & O’Connell, 2016, p. 8). Community management and reintegration can occur as a result of interaction with many settings which includes outpatient rehabilitation, primary care, specialist care, home care, community based programs, long term care and palliative care (Cameron & O’Connell, 2016).
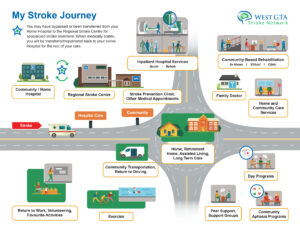
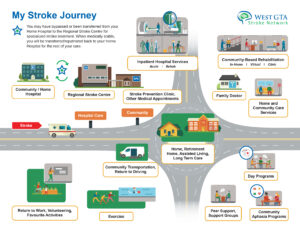
Leveraging the work of other stroke networks in the province, the West GTA Stroke Network undertook consultations with providers and persons with stroke to develop a visual patient journey map which highlights key services that may facilitate reintegration after stroke.
PROVINCIAL WORK ON COMMUNITY REINTEGRATION
Many regions around the province have undertaken work on community reintegration. Here are some examples:
-The Stroke Network of Southwestern Ontario conducted focus groups with providers, patients and family members to identify components that facilitate community reintegration. The findings of this engagement is available in a report titled Pathways for People with Stroke to Live Fully in the Community.
-The Stroke Network of Southeastern Ontario produced a report titled Building Capacity to Enhance Community Reintegration of People with Stroke which utilized regional and local forums to identify emerging directions and principles related to community reintegration. In 2015, The Stroke Network of Southeastern Ontario also conducted community wide consultations to hear stroke survivor, caregiver and health care provider voices to chart a course toward improved community reintegration. This report identifies priority areas for change as well as the resulting recommendations for charting that course.
-Outside of Ontario, the Stroke Recovery Association of British Columbia Developed the 7 Steps to Stroke Recovery which outlines steps that can be taken to overcome challenges as a result of a stroke.
CANADIAN STROKE BEST PRACTICE RECOMMENDATIONS AND INTERNATIONAL WORK ON COMMUNITY REINTEGRATION
An important update has been released for the Heart & Stroke Canadian Stroke Best Practice Recommendations (CSBPR) for Rehabilitation, Recovery and Community Participation. This module includes two parts:
- Part One: Rehabilitation and Recovery following Stroke
- Part Two: Transitions and Community Participation following Stroke Components of both of these modules are important to community reintegration. The full reports can be found here.
Another pivotal report on community reintegration post stroke was released by the Stroke Association UK. The Stroke Association UK Lived Experience Report (2019) was based on survey of over 10 000 persons with stroke and caregivers. The survey focused on areas where persons with stroke received support and areas in which they did not. Many aspects which impact community reintegration such as cognition, mental health, independence, relationships/social life, caregiver burden and ability to work are discussed in this report.
WEST GTA STROKE NETWORK COMMUNITY REINTEGRATION COMMITTEE
The West GTA Stroke Network has also undertaken important work in the area of community reintegration post stroke. In May 2019, the West GTA Steering Committee approved the formation of the Community Reintegration Expert Committee to explore the topic of community reintegration by identifying key community programs that are required to support persons with stroke after they completed their rehabilitation. The WGTASN Community Reintegration Expert Committee was made up of community providers currently offering community programs to persons with stroke in the West GTA Stroke Network.
As a part of the work of the Community Reintegration Expert Committee, a survey was developed for persons with stroke and providers to identify key community reintegration programs post stroke. In total, 216 surveys were collected between the two surveys. The Community Reintegration Expert Committee also reviewed key literature on community reintegration. Using the survey results and the literature the group made 12 recommendations. The recommendations were prioritized by the group. Feedback was also received from 6 persons with stroke/caregivers on the prioritized recommendations. The recommendations made by the group are meant to provide the groundwork necessary to advance community reintegration in the West GTA Stroke Network region. To see the recommendations please see the Community Reintegration Committee Executive Summary.
COMPLETED INITIATIVES RECOMMENDED BY THE WEST GTA COMMUNITY REINTEGRATION EXPERT COMMITTEE
Initiative 8: Aphasia Awareness
Last year, the West GTA Stroke Network Regional Community Reintegration Committee created a survey for persons with stroke, caregivers, and providers to identify key components of community programs. One common theme that was mentioned in the feedback from our region, is the need for improved cross continuum aphasia awareness. The community reintegration committee felt that one way to raise awareness about aphasia was to create a marketing campaign/infographic about aphasia and resources that are available. Thank you to the Halton-Peel Community Aphasia and Holly Sloan SLP at Trillium Health Partners for their assistance with this campaign.
Initiative 5: Resource Inventory
Initiative 3: Depression Post Stroke
Initiative 7: Peer Support
Stemming from the work of the Community Reintegration Expert Committee, a working group was formed to identify ideal peer support structure (timing, content, frequency) in our region using available evidence. The working group will also assist in examining the logistics of implementing peer support in communities that currently do not offer this service (Orangeville, Georgetown). The working group will examine the Canadian Stroke Best Practice Recommendations, Canadian literature and models of peer support from existing peer programs. The working group will also discuss the impact of the COVID-19 pandemic on the use of virtual technology to support peer support. The ultimate purpose of this work is to compile the available evidence to progress peer support in northern geography of our region. The full report from this committee is found here.
Initiative 6: Return to Work (Vocations)
Stemming from the work of the Community Reintegration Expert Committee, a working group was formed to examine the process of return to vocations (work, school, volunteering), supports, and employer obligations. The working group consists of members from the Central East and West GTA Stroke Networks. The work will include a literature review, review of the Canadian Stroke Best Practice Recommendations, a provider survey, and an adivsory group with persons with stroke. The deliverable for this intiative is a return to vocations resource that will be targeted at stroke care providers in the Central East and West GTA Stroke Networks. The work is set to be completed by March 2022. A current copy of the project charter can be found here.
OVERVIEW OF LONG-TERM CARE
One in five stroke survivors are admitted to complex continuing care or long term care settings. Most persons with stroke admitted to these settings don’t return back to the community after their stroke. The characteristics of persons with stroke residing in long term and complex continuing care settings has been highlighted in a report by CorHealth Ontario.
With over 50 LTC homes in the Mississauga Halton and Central West regions, our team is dedicated to promoting the use of stroke best practices within these facilities.
The Canadian Stroke Best Practice Recommendations on Transitions of Care highlight assessment, care planning, rehabilitation, restorative care, and education for persons with stroke and their families in the long term care settings.
Numerous resources have been compiled by our team to help support ongoing learning and development in the long term care sector.
ADDITIONAL LEARNING RESOURCES FOR LONG TERM & COMPLEX CONTINUING CARE STAFF
This page is a collection of resources that may be useful to staff taking care of persons with stroke in the long term and complex care setting.
One great resource for providers working in the long term care setting are the Stroke Care Plans. In June 2011, a collaborative project was developed between LTC Home representatives and Ontario Stroke Regional Community and LTC Coordinators (CLTCs) to integrate stroke best practices into long-term care facilities. The objective of this project was to link stroke best practice information with Resident Assessment Instrument –Minimum Dataset (RAI-MDS) data elements and Resident Assessment Protocols (RAPs) through the integration of best practice Stroke Care Plans into existing LTC care plan libraries. Twelve Stroke Care Plans were developed based on the Tips and Tools for Everyday Living© (Heart and Stroke Foundation of Ontario, 2010) best practice resource and incorporating RAI MDS Outcome Scales. As a result, the Stroke Care Plans translated evidence-based, best practice stroke care into comprehensive and practical care plans for front line providers. The updated Best Practice Stroke Care Plans for Long Term Care Homes are available on the CorHealth Ontario website . These care plans have been updated to reflect the new Heart and Stroke Foundation’s Taking Action for Optimal Community and Long-Term Stroke Care (2015) – a resource for healthcare providers caring for stroke survivors.
The Community & LTC Coordinator of the West GTA Stroke Network can help support your organization with the implementation of the Stroke Care Plans as well as other quality initiatives designed to provide LTC residents with care that reflects best practices.
Stroke Network of Southeastern Ontario: Blood Pressure Toolkit for PSW
This toolkit is designed to assist Personal Support Workers (PSW) and other health care team members to acquire the practical knowledge and skills to support blood pressure management and to build the capacity to work collaboratively with the health care team and resident/client to optimize blood pressure management. This program is meant to be individualized depending on the needs of the learner and in accordance with the employer/client’s guidelines. The Learning Plan is divided into two modules each of which can be used independently of the other (Module #1: The Basics of Blood Pressure & Supporting the Patient and Module #2: How to Take Blood Pressure). The toolkit may be used by educators or as self-learning modules.
- Learning Plan
- Module 1 “The Basics of Blood Pressure and Supporting the Patient” provides a theoretical overview of blood pressure including hyper- and hypotension, risks for hypertension, impacts of hypertension and role of the care provider.
- Case Studies (Module 1) – Three case studies have been developed to support learning. Each case study has a participant and a facilitator version. The case study questions are designed to demonstrate achievement of the evaluation criteria.
Oral Health Videos for Long Term Care
Members of the Seniors Health Research Transfer Network Oral Health Community of Practice produced 13 education webinar-based videos on various oral health topics for long-term care.
Stroke Network of Southeastern Ontario: The Brain, The Body, and You Workshop Series
This 4-session interprofessional, continuing education workshop series is designed for regulated and unregulated frontline care providers caring for stroke survivors and other complex client populations in the community, long-term care and other care settings. This continuing education program can be easily individualized by selecting the particular module(s) needed to meet the identified learning needs. It may be offered within existing academic settings or in other educational settings such as the workplace. The 4 modules are each 4 hours in length. The module topics include:
Facilitator Equipment Required
Stroke Care – Prevention to Life after A Stroke
Mobility
Nutrition, Swallowing, Feeding and Hydration
- Presentation & Speaker Notes – Currently being updated
Communication and Behaviour
- Communication Presentation & Speaker Notes
- Communication Materials
- Behaviour Presentation
You may use this education program within any existing educational settings or the workplace.
Southeastern Ontario Stroke Network: Tips & Tools for Everyday Living A Guide for Stroke Caregivers (Video Series)
Six education videos have been developed by stroke care champions in Southeastern Ontario. These videos are designed to complement popular sections of the Tips and Tools for Everyday Living: A Guide for Stroke Caregivers (2010) and education programs currently underway across Ontario and Canada. Five of these videos are designed for front line staff and one has been developed for family and community education.
Recognize & React to the Signs & Symptoms of Stroke for Health Care Providers
Communication
Meal Assistance & Hydration
Cognitive, Perceptual & Behavioural Problems
Mobility
Aphasia Institute Introduction to Supported Conversation (SCA™) eModule
This is a short self-paced online module. It is a prerequisite for Aphasia Institute workshops and is hosted on the Aphasia Institute Community Hub, an online platform that enables healthcare professionals to register for professional training and to join webinars.
STROKE PARTNERS DAY 2023
MY STROKE JOURNEY MAP
COMMUNITY BASED STROKE REHABILITATION
Community Stroke Rehabilitation refers to rehabilitation services received after discharge from the inpatient hospital setting. This part of the stroke continuum includes services received in the outpatient department and in home. The Canadian Stroke Best Practice Recommendations outline several recommendations on the core elements of community stroke rehabilitation services.
Rehabilitative Care Alliance also has a non-stroke specific definition of Community Based Levels of Rehabilitative Care which is broken down into “progression” and “maintenance streams”. Community Stroke Rehabilitation services after a stroke would fall into the “progression” category of this definition. Community reintegration programs conducted by allied health professionals would align with the “maintenance stream” (i.e. supportive communication programs). The Rehabilitative Care Alliance also has a useful listing of all of the rehabilitative care services in Ontario which can be found here.
Several important initiatives were also undertaken by the regional stroke networks. In 2015, work on identifying the available community stroke rehabilitation models in Ontario was undertaken. Specifically, the purpose of this work was to amalgamate the knowledge and lessons learned from the development, implementation, and successes of existing and emerging programs in an attempt to inform and guide the development of future models. The Community Stroke Rehabilitation Models in Ontario report was released by the Ontario Stroke Network on July 4, 2016.
Stroke rehabilitation in the community and outpatient setting was also identified as a provincial priority by the eleven regional stroke networks in Fall 2016. To address this priority, a working group from the stroke networks was formed and the resulting components of this work include:
1. A resource tool outlining methodology to do an estimate demands analysis for stroke outpatient/community rehabilitative services based on a region’s own geography.
2. Summary of common emerging facilitators and change ideas that outpatient (OP) programs have implemented to meet stroke best practices.
3. A decision making algorithm to assist clinical teams to determine what factors to consider when referring patients to existing programs.
These deliverables are now available on the CorHealth Ontario website.
EXERCISE POST STROKE
Physical exercise post stroke can help to lower a person’s risk of subsequent stroke. Participating in exercise classes within the community allows the stroke survivor to build a social network, reducing social isolation and improving community reintegration. Canadian Stroke Best Practice Recommendations on Transitions of Care (2019) highlight that people with stroke should be encouraged to participate in evidence-based community exercise programs.
Numerous resources are available to facilitate the implementation of quality community exercise programs for persons with stroke. One resource that is available is the Ontario Stroke Network Post Stroke Community Based Exercise Guidelines. This document considers many components of providing an exercise program for persons with stroke such as medical clearance, screening, class structure, supervision, exercise principles, program evaluation and much more.
Need help designing a program for stroke survivors? Numerous evidence based exercise programs have been designed for easy implementation. Some examples of already designed exercise programs include:
- The Together In Movement and Exercise (TIME™) program, developed by Toronto Rehab, is a community based exercise program for persons with balance and mobility issues. This program involves the joint cooperation of both the community organization and a licensed healthcare provider. A toolkit and license can be purchased online to assist you in starting up a TIME™ program in your community. The West GTA Stroke Network can help connect you with local healthcare providers who can assist with the training and running of the program.
- FAME is a community-based exercise program developed for people with stroke who have some standing and walking ability. This program has shown to improve mobility, cardiovascular fitness, arm and hand function post stroke. A physical therapist or occupational therapist instructed the patient in the program, but the patient did the program independently.
- The Nortwestern Ontario Stroke Network developed the Fitness Instructor Training Program: Community-Based Exercise for People Living with Stroke. This resource is an instructor training package in DVD format with the goal to provide a standardized, competency-based approach to training. Completion of the training program enables non-health care professionals to deliver an exercise program based on best practice to people living with stroke. This strategy is one way to utilize the expertise of physiotherapists, while more fully integrating community program into the continuum of stroke care.
- Graded Repetitive Arm Supplementary Program (GRASP) is a community-based group upper extremity program. This functional program of upper extremity strengthening, fine motor tasks and repetitive functional tasks has demonstrated improvements in arm and hand function (Chedoke Arm and Hand Activity Inventory, Action Research Arm Test), use of the hand (outside of therapy) and grip strength.
Strong evidence also exists to support the use of aerobic activity after stroke to improve walking speed and endurance, increasing exercise capacity, increasing muscle strength, reducing vascular risk, improving cognition, and emotional well-being. Health care providers should try to incorporate aerobic activity across the continuum of care. One resource available to providers to learn about incorporating aerobic activity is Aerobic Exercise After Stroke. An online module to support the implementation of the Aerobics Guidelines can be found here. A guide for persons with stroke about the benefits of aerobic activity titled How Aerobic Activity Can Help You After A Stroke is also available.
Some individuals attending an exercise class may have communication difficulties as a result of their stroke. The Aphasia Institute has numerous resources for providers to learn about supported conversations including the Supported Conversation eModule.
DRIVING POST STROKE
Motor, sensory, cognitive or visual impairments from stroke can limit a person’s ability to drive. Many persons with stroke have questions about return to driving after stroke. The resumption of driving is addressed in the Canadian Stroke Best Practice Recommendations Transitions and Community Participation Post Stroke Module (2019). These recommendations cover education, screening, assessment for fitness to drive, and rehabilitation for return to driving.
The West GTA Stroke Network Community Resource Booklet provides a list of service providers in the West GTA and surrounding areas that can help get clients back on the road. A full list of Driver Assessment Centers across Ontario can be found on the Ministry of Transportation Website.
Several additional resources are available on the topic of return to driving after stroke that are useful. These include:
- Southwestern Ontario Stroke Network Driving After Stroke in Ontario
- Stroke Engine Driving After Stroke
- Toronto Stroke Networks Planning for your Return to Driving
- BrainXchange Driving and Dementia e-learning module
- Southeastern Ontario Stroke Network Driving After Stroke Resource for Stroke Survivors and Families
RETURN TO WORK POST STROKE
Many persons with lived experience have questions on returning to work post-stroke. The West GTA Stroke Network and the Central East Stroke Network collaborated to create the Return to Vocations Post Stroke Toolkit for Providers. The purpose of the toolkit was to:
- support front-line providers in addressing recovery goals related to return to work, school or volunteering post stroke
- facilitate conversations on the topic of return to vocations post stroke in the Central East and West GTA Stroke Network regions.
There are several additional resources on the topic of return to work after stroke developed through the Ontario Stroke Networks. These include:
- Southwestern Ontario Stroke Network Return to Work Self Assessment Guide for People With Stroke
- Southeastern Ontario Stroke Network Return to Work Toolkit
RETURN TO VOCATIONS AFTER STROKE WEBINAR January 16th, 2026
On Friday, January 16, 2026, the West GTA Stroke Network, in collaboration with the Central East Stroke Network, hosted a Return to Vocations After Stroke webinar. Guest speakers Dr. Liza Pain, PhD, Occupational Therapist, and Paula-Jane Bellizzi, MSW, Social Worker, shared their professional knowledge and experience supporting individuals after stroke in returning to work, education, and other meaningful vocations.
A recording of the webinar and the presentation slides are available below.
Return to Vocations After Stroke Webinar Presentation Slides Jan 16 2026